This isn’t an atrial fibrillation link, per se, but I think it will be of interest to readers of afibrunner.com. In Wounded Heart Project Shane describes his journey from having a myocardial infarction at age 42 (and subsequent obesity) to changing and regaining his health via improved diet (whole food plant based diet – yeah!) and exercise eventually becoming a sub-four hour marathoner even though his ejection fraction remains at 37%! That’s inspiring to me – is it inspiring to you?
Afib Runner News Update – Vitamin D Helps with Heart Failure & Exercise Helps Atrial Fibrillation Outcomes
Vitamin D Helps with Heart Failure
I’m not certain this first item has much to do with readers of this blog – theoretically we are getting outside and getting plenty of sunshine, but a recent study showed that supplementation with high doses of vitamin D improved left ventricular structure and function in patients with chronic heart failure, although it doesn’t improve walking distance (citation below). I think the people in this study were a little worse off than a typical afib runner. In this study the non-placebo group received 4000 IU of vitamin D.
Personally, I like to supplement with vitamin D – one of two supplements that I take. I tested my vitamin D levels via a blood test several years ago and was at the low end of normal even with modest supplementation. This is interesting considering that I was running about 35 miles a week, all outdoors!
The other supplement I take is B complex – pretty standard for vegetarians.
Good news for fib runners: Exercise is good for your a trial fibrillation!
At the recent American College of Cardiology’s 65th Annual Scientific Session & Expo, findings were presented that show exercise reduces risk of cardiovascular death and all cause death. And it appears that the more you exercise the better the outcome.
I have a citation below, but I will summarize by saying that in a European study with over 2000 patients, subjects were divided into four groups based on weekly exercise: none (38.9%), occasional (34.7%), regular (21.7%), and intense (4.7%). In a two year follow up it was determined the “regular” and “intense” group had lower death rate, improved outcomes, etc. And of course the “intense” group did better than the “regular”, “regular” did better than “Occasional,” etc.
So there you go – justification for continuing to work out with atrial fibrillation. It seems obvious but it is nice to see proof.
Vitamin D and hearth failure:
Witte KK, Byrom R, Gierula J, et al. Effects of vitamin D on cardiac function in patients with chronic HF: the VINDICATE study [published online April 2016]. J Am Coll Cardiol. doi:10.1016/j.jacc.2016.03.508.
Exercise and afib:
Proietti M, Boriani G, Laroche C, et al. Physical activity and major adverse events in patients with atrial fibrillation: A report from the EURObservational research programme pilot survey on atrial fibrillation (EORP-AF) general registry. Paper presented at: 65th Annual Scientific Session & Expo; April 4, 2016; Chicago, IL. http://www.abstractsonline.com/pp8/#!/3874/presentation/42867.
Runners with Atrial Fibrillation – Considering the Watchman?
Are you considering the Watchman device?
Ever since having a TIA/stroke, I certainly have thought a lot about it.
What is it? The Watchman, by Boston Scientific is a little device, sort of like a basket, that can be inserted into the left atrial appendage, theoretically blocking it off and preventing clot formation. As you probably know already, clot formation may lead to Stroke. The device was FDA approved in the US in March, 2015, and has been used in Europe since 2005.
It’s placed in the left atrial appendage via a catheter through an artery in the groin, and if all goes well the patient can discontinue their blood thinner (warfarin, etc.) within six months.
Sounds great, doesn’t it?
I know I’d love to be protected from having another TIA or stroke and not have to take a blood thinner – I’m currently on warfarin + aspirin which makes bicycling, especially mountain biking, quite hazardous. But truthfully, it’s not that I necessarily want to be off the warfarin: I just don’t want to ever have another TIA/stroke. Recall that I had my event while I was already taking Pradaxa (and I never missed a dose). I just want a treatment that is going to work.
But there is some evidence to suggest the Watchman might not be as terrific as it sounds.
A recent study showed that the risk of a major bleed over the course of three years is the same with the Watchman compared to just staying on warfarin. Huh?
This is an excerpt from a Medscape article:
Patients with atrial fibrillation (AF) who received a left atrial appendage closure device (Watchman, Boston Scientific) or stayed on long-term warfarin therapy had similar rates of major bleeding during a mean follow-up of 3.1 years, in pooled analysis of two randomized clinical trials[1]. However, patients who received the device and were able to stop taking warfarin and clopidogrel at 6 months had lower rates of major bleeding from then onward, compared with patients receiving long-term warfarin.
Furthermore, in a very thoughtful, somewhat technical, article CMS Proposal on Watchman Is the Right Decision, Dr John Mandrola, a thought leader in Cardiology and Electrophysiology, agrees with the CMS proposal that “the evidence is sufficient to determine percutaneous left atrial appendage closure therapy using an implanted device is not reasonable and necessary.”
There are two major studies in the US regarding the Watchman. According to Dr Mandrola in the PREVAIL study, “Due to an excess of ischemic strokes, Watchman did not reach noninferiority in this category in the updated analysis presented to the FDA.” In PROTECT-AF study, “ischemic strokes were numerically higher in the Watchman group.” Which, ultimately, “leads one to conclude that the device is not effective.”
As for me, personally, as much as I’d like to believe the Watchman is a solution for me, the evidence, so far, is not convincing. I’m going to wait.
By the way, if any readers have experience with the Watchman PLEASE leave a comment below. We would love to hear from you!
Adverse effects of the Watchman:
“The main adverse events related to this procedure are pericardial effusion, incomplete LAA closure, dislodgement of the device, blood clot formation on the device requiring prolonged oral anticoagulation, and the general risks of catheter-based techniques (such as air embolism). The left atrium anatomy can also preclude use of the device in some patients.”
By the way – I linked a couple of articles from Medscape. I’m not certain but I think you need to be registered for that sight. Sorry.
Warfarin Withdrawal in Patient’s Awaiting Surgery Increases the Risk for Stroke
Last April Dr. Adnan I. Qureshi reported on research, at the 67th Annual Meeting of the American Academy of Neurology, that has shown that atrial fibrillation patient’s who are taken off of warfarin for surgical procedures have an increased likelihood of having a stroke.
Subjects included in the analysis had atrial fibrillation plus at least one additional risk factor for stroke or death: age >65 years, systemic hypertension, diabetes, congestive heart failure, transient ischemic attack, prior stroke, left atrium diameter 50+ mm, left ventricular fractional shortening <25%, or left ventricular ejection fraction <40%.
Specifically atrial fibrillation patients who discontinued warfarin for surgical procedures had a 1.1% rate of stroke while atrial fibrillation patients who remained on warfarin had a 0.2% rate of stroke.
Read more here:
Warfarin withdrawal in atrial fibrillation patients awaiting surgery dramatically ups stroke risk
Well, this seems like one of those articles where you read the headline and think, “Duh!” Like the article about how obese children have a higher chance of hypertension – No kidding?
Obviously if you are on a medication, in this case warfarin, to prevent having a stroke, and you stop taking the medication, well, you have an increase likelihood of having a stroke. I think everybody suspected this – but what we see here is that the rate of stroke increases five-fold. Wow – that seems incredible!
This article reinforces my strong belief that strict compliance with taking my medications, especially warfarin, is a good idea!
As far as surgery is concerned, clearly, if you need to have the surgery and you need to go off the warfarin, then so be it. The article didn’t mention anything about bridging with Lovenox. You might want to ask your surgeon about that. And also – consider how important the surgery is to your general health. Is the surgery truly necessary? Is it worth risking a stroke?
Runners with Atrial Fibrillation – Thinking About Having a Cardioversion? “Look Before You Shock”
This is, so far, the most discouraging article about atrial fibrillation I have ever read:
As a distance runner with atrial fibrillation, who never missed a single dose of my anti-coagulant, and who has already had a blood clot in my left atrial appendage, and has already had a “mini-stroke” – this one leaves me feeling a bit hopeless.
Feel free to read the article; but I will go over a few key points here. One of the dreaded consequences of atrial fibrillation is having a stroke. Because the top chambers of the heart, the atria (plural of atrium) are beating so fast that they are basically just sitting there vibrating, the blood pools and becomes sluggish, and is prone to forming blood clots. Combine this with an enlarged left atrium and the likelihood is even higher. The blood clot forms in a little corner of the heart called the “left atrial appendage” (LAA).
That’s where I formed a clot. If the blood clot, or a piece of the clot, breaks off it can quickly travel to the brain, get caught and cut off the circulation to part of the brain. This is a type of stroke, and is a huge problem for people with atrial fibrillation.
There are people who like to refer to a stroke as a “brain attack” because that’s what it is – like a heart attack in the brain. And like heart attacks there are big ones and small ones. I had a small one (TIA – tangent ischemia episode) that fortunately only lasted a minute or so. A big stroke, of course, can be fatal.
Important point: if a person is in atrial fibrillation and has blood clot in the LAA, it might be very stable. It might be just sitting there, hanging out, because the atria isn’t doing any beating. Everything is pretty tranquil in there. But then the person has a cardioversion (shock to reset the beating heart) or an ablation and the atrium begins to beat again, the blood starts moving through more quickly – well – now there’s a problem. Now the clot can break loose and BLAM!! – you’ve had a stroke!
The problem: it’s difficult to tell whether or not a patient has a clot prior to having a procedure. A regular echocardiogram doesn’t even show a small clot; there’s not enough detail. The best way to determine if a clot is present is to do a transesophageal echocardiogram (TEE).
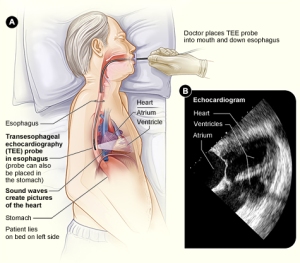 Transesophageal Echocardiogram
Transesophageal Echocardiogram
I’ve had three TEEs – it’s not fun – sort of like swallowing a telephone. Thankfully the last two that I had involved an anesthesiologist who put me to sleep for the procedure.
As far as I know it is fairly common to have a TEE prior to having an ablation procedure; but less common before a cardioversion (the shock!), especially for people who presumably have a low risk of a LAA blot clot – like people who are appropriately anti-coagulated, or people who have had atrial fibrillation for less that 48 hours.
In this article five interesting cases are reviewed.
Case #1 – a patient who was effectively anti-coagulated but turned out to have a LAA clot anyway (sounds familiar).
Case #2 – a patient who was actually more anti-coagulated than thought necessary, and was in atrial flutter for less than 48 hours, but turned out to have a LAA clot anyway.
Case #3 – an appropriately anti-coagulated person with a low risk of clot (CHADS2 score=1), but turned out to have a LAA clot anyway.
Cases #4 and #5 were high risk patients who would be expected to have a high risk of a clot. Case #5 actually had three clots in her heart – yikes!
How does all this apply to athletes with atrial fibrillation? Well, apparently healthy, athletic patients, who are appropriately anti-coagulated, and either undergoing a planned or emergency cardioversion, still have a certain risk of having a LAA clot and subsequent stroke.
Should everybody have a TEE before having a cardioversion? Probably not. TEE is expensive, unpleasant, and if anesthesia is involved it basically takes up an entire day out of your schedule. It might be a good idea to talk it over with your cardiologist, however.
What is the ACLS Approach to Atrial Fibrillation? (Advanced Cardiac Life Support)
A week or so ago I re-certified in ACLS – Advanced Cardiac Life Support. ACLS is a set of emergency clinical interventions for cardiac arrest, stroke, respiratory arrest, etc., which is basically a step above BLS (Basic Life Support – formerly known as CPR). ACLS certification, in my case anyway, is done through the American Heart Association, and is only open to health care providers: doctors, nurses, dentists, advanced practice providers like PAs and nurse practitioners, EMTs, respiratory therapists, pharmacists, and so on.
I thought I’d write about it in this blog so people might know what to expect as far as the type of treatment they might experience if they have an unstable episode of atrial fibrillation.
I’m in permanent atrial fibrillation, so when I’m in one of these classes I’m glad I’m not hooked up to an EKG – I don’t feel like getting medicated or shocked!
ACLS deals with various problems using algorithms, so let’s look at the “Tachycardia with a Pulse Algorithm” which would generally apply to acute atrial fibrillation.
So basically we start with a person with a fast heart rate. Tachycardia is, by definition, a pulse over 100 beats per minute, but for ACLS purposes it generally means a pulse over 150 bpm. Obviously not all tachycardia (fast heart rate) is atrial fibrillation.
For this article I am not discussing the other types of tachycardia, even though they are in the algorithm. I assume most people reading this blog are dealing with atrial fibrillation.
The first step is to assess the patient, identify and treat any underlying cause, make sure the patient is breathing effectively, assist if necessary, and give the patient some oxygen.
Now the next step is very important – is the patient stable? Five things: 1.) Is the blood pressure too low? 2.) Is there altered mental status (confusion)? 3.) Is the patient going into shock? 4.) Chest pain? 5.) Heart failure?
Even though I am in atrial fibrillation, all the time, I don’t have any of these symptoms. But if the patient is unstable and have tachycardia, basically, they are going to be getting some electricity! That means synchronized cardioversion, and in the case of atrial fibrillation (see “narrow irregular”) that means 120-200 joules – that’s a big shock!
Check out this video of cardioversion for atrial fibrillation – yikes!
Notice that it says “consider sedation.” Sedation can be considered, but not if it interferes with getting the unstable patient shocked as soon as possible. If you go into unstable atrial fibrillation at a race expect that the sedation will likely be skipped and get ready to be ZAPPED.
This is for unstable tachycardia – that means the patient is in some sort of crisis that may eventually be life threatening.
For an episode of stable atrial fibrillation expect vagal maneuvers and a referral to a cardiologist. Vagal maneuvers include firm carotid sinus massage, coughing, gagging, valsalva maneuver (holding your breath and “bearing down”), and placing your face in ice water (snow also works). A lot of people with intermittent atrial fibrillation already know how to do this.
For a great article about her episode of unstable atrial fib see Run, Smile, Drink Water and Don’t Die – A Guest Post by JoAnna Brogdon.
I’d be very interested in anybody else’s experience with unstable atrial fibrillation and what type of treatment was administered. Please comment below. Thanks.
Does Drinking Coffee Cause Atrial Fibrillation?
It has often been said that drinking coffee is related to developing atrial fibrillation. How about people who already have a history of atrial fibrillation? Can coffee trigger an episode?
A recent large study from Sweden shows that coffee consumption does not increase the chance of developing atrial fibrillation, even if quite a bit of coffee is consumed.
So coffee does not cause atrial fibrillation; not in people who have no history of atrial fibrillation.
But what about people who already have a history of atrial fibrillation? Can coffee trigger recurrence of atrial fibrillation?
The answer to that is probably yes, but more research needs to be done. In this study it was found that people who already had atrial fibrillation tended to drink less coffee than people without atrial fibrillation – probably to prevent triggering the arrhythmia.
As for me, I’m in permanent atrial fibrillation and it really doesn’t make much difference – I drink my normal amount of coffee and don’t worry about it.
Here are some excerpts from an article, by Colleen Mullarkey, in Consultant360:

After analyzing data from nearly 250,000 individuals, researchers found no association between coffee consumption and an increased risk of AF, according to the findings in BMC Medicine.
“This is the largest study to date on coffee consumption in relation to risk of atrial fibrillation,” says lead study author Susanna C. Larsson, PhD, associate professor in the Institute of Environmental Medicine at Karolinska Institutet in Stockholm, Sweden.
Larsson and her colleagues investigated the association between coffee consumption and incidence of AF in two prospective cohorts who had provided information on coffee consumption in 1997 and were followed up for 12 years—41,881 men in the Cohort of Swedish Men and 34,594 women in the Swedish Mammography Cohort.
Using the Swedish Hospital Discharge, they identified 4,311 and 2,730 incident AF cases in men and women, respectively, in the two cohorts. The median daily coffee consumption was 3 cups among both men and women.
In their analysis, the researchers found that coffee consumption was not associated with AF incidence, even in more extreme levels of coffee consumption.
They confirmed this lack of association in a follow-up meta-analysis that included both of these two cohorts along with four other prospective studies, which amounted to a total of 10,406 cases of AF diagnosed among 248,910 individuals.
“These findings indicate that coffee consumption does not cause atrial fibrillation,” Larsson says. “However, high coffee consumption may still trigger arrhythmia in patients who already have atrial fibrillation.”
While the researchers could not examine this possibility in the present study, they observed that participants who had AF at the time they completed the questionnaire about their coffee consumption drank, on average, less coffee (mean of 2 cups/day) than those who did not have atrial fibrillation (mean of 3 cups/day).
Data in the study suggests that some individuals who had AF at the start of the study may have quit drinking coffee or cut down their consumption because of an arrhythmic-triggering effect.
“Further study is needed to assess whether coffee consumption may trigger arrhythmia in patients with atrial fibrillation,” Larsson says.
Larsson SC, Drca N, Jensen-Urstad M, Wolk A. Coffee consumption is not associated with increased risk of atrial fibrillation: results from two prospective cohorts and a meta-analysis. BMC Med. 2015 Sep 23;13(1):207.
Now the next question: Does running really ruin your knees? (Ha ha)
afibrunner.com – Healthline’s The Best Atrial Fibrillation Blogs of the Year
I’m going to “ring my own bell” here and post that afibrunner.com has been chosen, once again, as one of Healthline’s The Best Atrial Fibrillation Blogs of the Year. Thanks so much, Healthline!
According to my WordPress dashboard I have a lot of views of my blog directed from healthline.com – I truly appreciate it.
Please feel free to leave comments on this blog.
Update Part 2 – Atrial Fibrillation, Pradaxa Fail, Transient Ischemic Episode, Blood Clot in Left Atrial Appendage
Jimi Hendrix sang, “manic depression’s a frustrating mess.” Well, I think the same can be said of atrial fibrillation!
 Ringo and Me – Photo by Ben Vallejos
Ringo and Me – Photo by Ben Vallejos
It’s been a while since I have written and I have to say the last couple of months have been nerve-wracking. As I posted in a previous entry I had a TIA (transient ischemic attack) while running a couple of months ago, had a normal carotid scan, but a TEE (trans-esophageal echocardiogram) showed that I had a small blood clot in my left atrial appendage.
In other words I had a “mini-stroke” and was at risk of having a full on stroke.
This TIA occurred while I was on Pradaxa, a newer, novel anticoagulant. At that point I was taken off Pradaxa, started on Lovenox (low molecular weight heparin) injections, and warfarin (Coumadin), and also aspirin. I was instructed to discontinue running, and bicycling, and limit my activity to easy walks, and a repeat TEE was scheduled two months after the initial one.
I won’t hold back any longer regarding the surprise ending – I never had a second TIA “mini-stroke” (that I know of) or stroke and the follow-up TEE (trans-esophageal echocardiogram) showed that the blood clot inside my heart is now gone. Hooray!
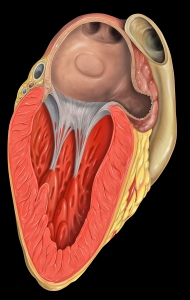 Photo – The little cul-de-sac is the LA appendage
Photo – The little cul-de-sac is the LA appendage
Just to review how this happens: when you are in atrial fibrillation your atria is beating so fast it’s like it isn’t beating at all, just sort of vibrating. There is a part of the left atrium (the “appendage”) where the blow flow is extra sluggish, and this is where clots can form. When a tiny piece of clot breaks of and goes into the brain that’s a TIA. If a big clot is present and breaks of into the brain that’s a stroke, which of course can be disabling and even fatal.
It goes without saying that I am disappointed that this occurred while I was on Pradaxa. I figured that as long as I was taking it I was safe, and I liked not having to watch my diet or have blood tests constantly. Taking Pradaxa is easy – “set it and forget it.” Now I’m on warfarin (Coumadin), a royal pain in the butt, and have to micromanage my diet constantly – this drug is not an easy choice for a vegetarian! Eating too many greens (think kale) is dangerous as is not eating enough greens. Imagine trying to eat about the same amount of kale or broccoli or spinach each day.
My target INR is between 2.0 and 3.0, but seeing as I have had a TIA while on an anticoagulant I am trying to keep it nearer to 3.0 or even higher (3.0 – 3.5).
The two months between echocardiograms was an era of angst – anxiety and fear – for me, especially the first several weeks. Every symptom, no matter how minor, seemed like stroke. For example – lie in bed trying to get to sleep and your hand becomes numb – normal, right? Not when you know you have a blood clot in your heart – that seems like a stroke! Jump up from bed, start testing the muscle strength in each arm and leg, recite the alphabet, smile, frown, move eyebrows up and down checking for asymmetry. Do you think I’m exaggerating?
Every once in a while a person stammers or mispronounces a word. Normal? Maybe, but not when you are obsessed with a gigantic blood clot lodging in your brain.
As far as exercise was concerned at first I was limiting myself to short, easy walks more appropriate for a non-athlete. Eventually I became a bit bolder and started doing longer (but slow, especially up hills) hikes of an hour or two. It took me three weeks (!) to bridge to a therapeutic INR, so I was on warfarin and Lovenox for all that time. Once I was off the injections I started doing bike rides – but they were on non-technical trails and were slow, especially while going uphill.
My brain never got the memo that I was no longer a long distance runner/cyclist so I still ate like I was, and consequently I’ve gained some weight.
At this point, after finding out the clot is no longer present, I have started increasing the intensity of my bike rides, but mostly I’m still doing bike rides. I haven’t yet started running again – but I will.
I am mountain biking again, but not on any trails that would be considered challenging. Well, that’s not 100% true, I guess.
 Photo – “Adventure Without Limits?”
Photo – “Adventure Without Limits?”
As far as mountain biking is concerned I am phasing out technical trails (gradually). I made a deal with my self that if I didn’t have the blood clot on the second TEE I would get a new bike – and I did. I got a Specialized AWOL, which is a “gravel grinder.” That’s sort of a cross between cyclocross bike and a loaded touring road bike – basically a bike designed for gravel or dirt roads – we have an infinite supply of these around here so I have a lot of exploring ahead of me.
As far as that blood clot is concerned I’m very pleased it has gone away – but I am not fooling myself that it is gone forever. It could return at any time. It wasn’t there when I had my second TEE, but it could actually be there right now – how would I know? How long had it been there and how many times have I had a clot in that area? There’s no telling without doing a ridiculously expensive, somewhat invasive test over and over. I guess all I can do is stay vigilant, take my meds, watch the diet, and keep on trying to run, hike, and ride, even if it is at a reduced level.
What Does Atrial Fibrillation Feel Like?

Some of the people who comment on this blog seem astounded that I can still run and bike while in atrial fibrillation. This surprises me because, at this point, I feel fine. Frankly just being on a relatively high dosage of a beta blocker (Carvedilol) is much more of a hindrance to my running than being in atrial fibrillation is.
But the big difference is that I am in permanent (constant) a fib. I’m used to it. And since I started taking the beta blocker I barely even notice the irregular beat. I’m slow now, and I get light-headed when I get up, but that’s it.
But recently I read a thread on a Facebook group, Atrial Fibrillation Information Exchange, and it was a real eye opener. I have forgotten how much other people suffer with atrial fibrillation. Here is a sample of comments (with spelling corrections) left in response to thread that asked:
Wondering what symptoms you get when in afib? What others feel and deal with?
-Rapid heart rate (220+), chest pressure/pain, dizzy, irregular heart beat, feel like I am going to lose consciousness.
-First my face feels warm,then the heart starts jumping erratically, can’t take an accurate pulse-then I know!
-I get a breathlessness, my rate stays low though but the overall feeling is like anxiety or the way one would feel before giving a speech or before competing in an athletic event etc.
-Mine is rapid heart rate,palpitations and anxiety
-All of the above plus hot and cold and violent vomiting. Also, if I’m sick, vomiting can bring it on
-Feels like there is a fish swimming in my chest, also weak and dizzy.
-Sweated and like your going to pass out , irregular and rapid heart beat , drinking cold water will help me convert, after I’m exhausted even will fall asleep haven’t had one in a few years now
-Like a squirrel doing back flips in my chest
-Felt like an anxiety attack plus tight feeling in throat( like it was dry and closing up) made me cough. Light headed/ dizzy, tired.
-I’ve had 8 AFib episodes since June of 2011. It always happens when I come out of a state of rest and stand up and start to walk. Except last month all I did was hiccup and cough at the same time and it triggered my AFib. Went to the ER and had cardioversion. I’ve never felt sick, dizzy, sweaty, breathless, nothing. Just racing heartbeat with strong palpitations.
-Mine was accidentally diagnosed initially on a routine office EKG.
-I get a “sinking” feeling in my chest.
-Flopping in my chest, weak, nausea, panic, sweaty, very very uncomfortable.
-I never come out of AFib. I had a stroke 5 years ago that affected my left side. I developed central pain syndrome in my left arm. So my heart sort of hurts and I have pain in my left arm.
-Weak breathless chest tight
-I had no symptoms other than lack of sleep and then the symptoms that go along with that. And symptoms from the meds. Oh, and the stroke.
-Sometimes it’s real quick flutters, or a skipped beat, I feel weak, sluggish, my chest hurts a little, and sometimes I get flushed and feel real anxious and nervous for awhile.
-Anxious & funny feeling in chest
-It’s almost like it’s gonna be an anxiety attack, but never goes to one thank goodness
-I have had episodes so bad I thought I would die. Then while in a fib, having to urinate every five minutes. It was like my body was in total rebellion. Sudden movements can trigger. Stress is a biggee.
I need to consider myself fortunate that I am so stable and feel so normal in permanent atrial fibrillation. I can recall what it was like when I was in sinus rhythm and would go into atrial fibrillation, usually during a long run, or even during a marathon – this is how I felt: I felt like crap – weak, mild malaise, light-headed, with vague chest and shoulder pain with exertion. Not pleasant by any means.
I’m curious – how do other fib runners feel while in atrial fibrillation? Please feel free to comment below.
















