This is, so far, the most discouraging article about atrial fibrillation I have ever read:
As a distance runner with atrial fibrillation, who never missed a single dose of my anti-coagulant, and who has already had a blood clot in my left atrial appendage, and has already had a “mini-stroke” – this one leaves me feeling a bit hopeless.
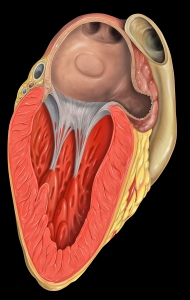
Feel free to read the article; but I will go over a few key points here. One of the dreaded consequences of atrial fibrillation is having a stroke. Because the top chambers of the heart, the atria (plural of atrium) are beating so fast that they are basically just sitting there vibrating, the blood pools and becomes sluggish, and is prone to forming blood clots. Combine this with an enlarged left atrium and the likelihood is even higher. The blood clot forms in a little corner of the heart called the “left atrial appendage” (LAA).
That’s where I formed a clot. If the blood clot, or a piece of the clot, breaks off it can quickly travel to the brain, get caught and cut off the circulation to part of the brain. This is a type of stroke, and is a huge problem for people with atrial fibrillation.
There are people who like to refer to a stroke as a “brain attack” because that’s what it is – like a heart attack in the brain. And like heart attacks there are big ones and small ones. I had a small one (TIA – tangent ischemia episode) that fortunately only lasted a minute or so. A big stroke, of course, can be fatal.
Important point: if a person is in atrial fibrillation and has blood clot in the LAA, it might be very stable. It might be just sitting there, hanging out, because the atria isn’t doing any beating. Everything is pretty tranquil in there. But then the person has a cardioversion (shock to reset the beating heart) or an ablation and the atrium begins to beat again, the blood starts moving through more quickly – well – now there’s a problem. Now the clot can break loose and BLAM!! – you’ve had a stroke!
The problem: it’s difficult to tell whether or not a patient has a clot prior to having a procedure. A regular echocardiogram doesn’t even show a small clot; there’s not enough detail. The best way to determine if a clot is present is to do a transesophageal echocardiogram (TEE).
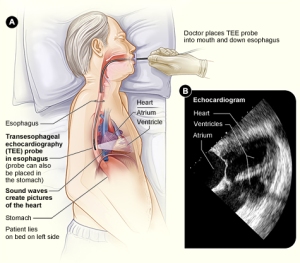 Transesophageal Echocardiogram
Transesophageal Echocardiogram
I’ve had three TEEs – it’s not fun – sort of like swallowing a telephone. Thankfully the last two that I had involved an anesthesiologist who put me to sleep for the procedure.
As far as I know it is fairly common to have a TEE prior to having an ablation procedure; but less common before a cardioversion (the shock!), especially for people who presumably have a low risk of a LAA blot clot – like people who are appropriately anti-coagulated, or people who have had atrial fibrillation for less that 48 hours.
In this article five interesting cases are reviewed.
Case #1 – a patient who was effectively anti-coagulated but turned out to have a LAA clot anyway (sounds familiar).
Case #2 – a patient who was actually more anti-coagulated than thought necessary, and was in atrial flutter for less than 48 hours, but turned out to have a LAA clot anyway.
Case #3 – an appropriately anti-coagulated person with a low risk of clot (CHADS2 score=1), but turned out to have a LAA clot anyway.
Cases #4 and #5 were high risk patients who would be expected to have a high risk of a clot. Case #5 actually had three clots in her heart – yikes!
How does all this apply to athletes with atrial fibrillation? Well, apparently healthy, athletic patients, who are appropriately anti-coagulated, and either undergoing a planned or emergency cardioversion, still have a certain risk of having a LAA clot and subsequent stroke.
Should everybody have a TEE before having a cardioversion? Probably not. TEE is expensive, unpleasant, and if anesthesia is involved it basically takes up an entire day out of your schedule. It might be a good idea to talk it over with your cardiologist, however.



Hi
I was looking for information on Atrial Fibrillation today when I came across your excellent site and article: Runners with Atrial Fibrillation – Thinking About Having a Cardioversion? “Look Before You Shock”
Great stuff !!
Actually, I just put together an info-graphic about AFIB. As someone that likes to write about AFIB, I thought you might get a kick out of it.
Let me know if you want to check it out.
Cheers!
Janco Vorster
Thanks for your kind words. I’ll go ahead and write an article and link to your blog, also, I’d invite you to write be a guest blogger on this blog and share your experience.
I just found your blog and I thank you for the information. I am 57 years old and have run multiple marathons and have had three TIAs/Strokes during the last three years and I have now been diagnosed with AFib. I had a cardioversion yesterday, so I will see how it affects my activities.
I am taking Eliquis after having taken aspirin for a year and a half only to suffer a TIA in February.
Thanks for yr kind words. Best wishes – and please let me know if you’d like to write a guest blogger article. I would appreciate your experiences.
I would be happy to contribute. Let me know what ty of information you would like. My cardioversion did not hold. We are going to try again.
My doctor gave me a TEE as a the last test in a long line.They were looking for the cause of the TIA. The test was helpful in that it located the probable cause to be a PFO. I found it funny(but not) that the test in itself could cause a stroke!! At least that was listed in the information I was given before the test. Two years later I am having flutter issues and the doctor just prescribed plavix. I refused any of these because I run by myself and didn’t want an extra problem of not being able to stop the bleeding if something happened. I have been taking an aspirin though and it has been fine. I read yesterday that NSAIDS are off limits with Plavix. Uh, I don’t know anyone who doesn’t take OTC meds especially active people. Did you have any issues with your drug and NSAIDS? I am trying to find information before I take that first dose.
Clearly this is an issue you need to discuss and come to an agreement with your physician. As for me – I haven’t taken any ibuprofen, or any other NSAIDs (other than my low does aspirin) since I’ve been anticoagulated. The reason is that I don’t want to increase my chance of a GI bleed. I understand that many runners take ibuprofen nearly daily – but I never have been like that. Even before I had any a fib problems I avoided it because it does bother my stomach. It’s frustrating and there is no good choice, really – you need to weigh the chance of a stroke with the chance of a bleed.
Having a TOE ( as we call it in the Uk) and having to take a day off versus having a stroke and having the rest of your days off? Surely a no brainer?
I had a TOE and cardio version today. All good so far.
Pingback: Cycling and AF Blog | A Fib Runner – Distance Running and Mountain Biking With Atrial Fibrillation